Industry Thought Leadership
Unleashing the Power of Digital Health
September, 20171. Driving better outcomes in healthcare: a global objective
It is widely recognized today that the global health and healthcare system is ill-equipped to deal with the demographic transformation (by 2050, the world’s population is expected to rise to 9.7 billion, with 2 billion over the age of 60). The United Nations 2030 agenda for Sustainable Development has defined 17 Sustainable Development Goals (SDGs) including SDG 3 for health which aims to ensure healthy lives and promote well-being for all at all ages. To keep populations healthy, treat patients more effectively, and attain the SDG targets, the traditional healthcare requires a profound transformation to move to value based care, drive better outcomes, lower cost, and enhance the delivery of healthcare globally.
2. The value of digital health
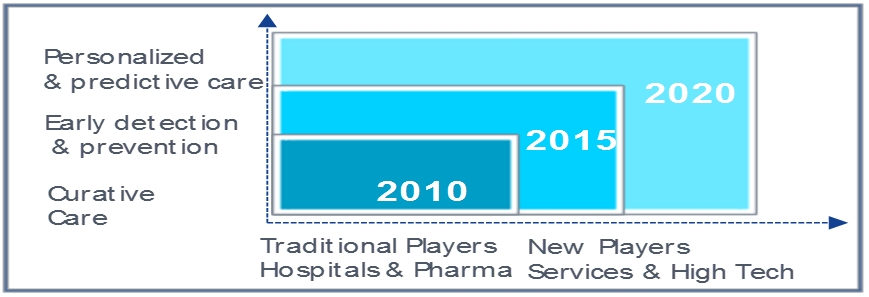
Nokia believes that digital health will revolutionize the concept of health care, from a technological and social standpoint and beyond, and will transform the ‘doctor-hospital’ model. Healthcare professionals will continue to monitor patients, but patients will be empowered to take their healthcare needs into their own hands. Advanced digital technologies such as connected health and well-being devices and sensors, IOT (Internet Of Things), Ultra-broadband connectivity networks, and the Cloud can help healthcare organizations work more efficiently, reach more patients, and gain deeper insight into both individual and population health trends and patterns. Digital health is a horizontal enabler for many global initiatives such as advancing the NCD (non-communicable diseases) agenda, containing global disease outbreaks and future epidemics, etc. As the digital health care ecosystem matures and solutions scale up, preventive care, early intervention, and personalized predictive care will take a center stage, reducing spending on chronic conditions and on high-cost emergency room visits, bringing efficiency and quality of health care to all. As a matter of fact, remote monitoring can now be done cost-effectively, because devices benefit from industrial volumes, connectivity is becoming more accessible, and artificial intelligence tells the clinician exactly where to look. From a modest 60 patients per nurse at the time hypertension was followed by phone, care coordinators can now follow hundreds of patients each digitally, a ten-fold productivity increase. This is not a futuristic vision. It is happening now in major healthcare institutions thanks to Nokia’s technologies: in the US (at Kaiser Permanente, Ochsner Health Systems, Duke Hospitals), but also at the Leiden Hospital in the Netherlands, and in the UK with the National Health Service. They are using Nokia’s new Patient Care Platform, allowing doctors and care teams to remotely monitor patients via their smart devices.
3. How to unleash the power of digital health?
The Health sector needs to unleash the power of technology to fundamentally reinvent how care is delivered. While considerable success has been achieved demonstrating how digitalization and the adoption of digital health can improve health services delivery, most achievements consisted so far in pilot programs and small scale initiatives. In order to integrate digital health interventions as part of the global health service delivery, and attain large scale digital health impact, both public and private sectors need to collaborate and embrace a digitally enabled care by driving some of the key actions described here next:
- Promote Investment in good and reliable infrastructure to bring better and faster healthcare for all. Evolutions to ultra-Broadband technologies such as 5G, IOT, and Cloud are examples of technologies driving innovation. Nokia is working with Finland’s Oulo University Hospital on becoming the world’s first 5G hospital. It is a test lab for trials of new devices and equipment that will help doctors make faster, more reliable diagnosis with the help of data analysis.
- Provide proper training/awareness building to health professionals and patients alike to encourage greater adoption of digital health solutions. Ensure continued investment in experimentation and certification demonstrating the efficacy of digital healthcare innovations.
- Reassure doctors and patients about connected devices and sensors. Devices for medical use must be certified before being introduced on the market. Also, the explosion of connected health applications in the market will pose a true challenge for health authorities. At the same time, the regulatory framework today makes a distinction between regulated and unregulated health devices. It’s important to keep a clear differentiation to enable new innovative solutions to flourish.
- Enable Big Data analytics. Huge amount of data is created by the health information systems that need to be easily accessible in a consistent manner. Digital health data integration with Electronic Health Records is necessary, to establish data repositories allowing for Big Data analytics to generate novel insights into citizens’ health status, disease progression and management, public health and personalized healthcare. Research teams in the United-States and Europe are now studying how Nokia wearable devices can help detect exacerbations from patients suffering from Multiple Sceloris (MS) and Cystic Fibrosis (CF). While these two diseases are very different, both studies aim to test how patient self-monitoring using a wide array of sensors can help detect and better manage exacerbations. Studying alerts can help clinicians develop a patient’s personalized educational plan, enabling better management of exacerbations, including ability to make informed choices.
- Invest in experimentation and evaluation. Nokia teamed up with the American Medical Group Foundation (AMGF) as an example to work on an 18-month project seeking to improve blood pressure control in patient with uncontrolled hypertension, in conjunction with the national Measure Up/Pressure Down® hypertension campaign. Also, in association with the French National Railway company, Nokia organized a public challenge around physical activity, which recruited 6200 members who tracked their steps for a period of 10 weeks. These same participants were asked to participate in a public health study, aimed at assessing the real impact of public transports on physical activity.
- Reassure about data protection. Medical data is sensitive personal data. It is essential to reassure users and doctors about the security and privacy of the data and associated solutions. The status of data changes depending on whether the device is used for recreational purposes, in which case it’s personal data, or in a medical context, in which case it requires conformity to specific hospital norms. The relevance of the collected data is not the same depending on whether the individual uses it himself or not. In the first case, it is the patient’s own responsibility. When a doctor uses data, he is held responsible for it and for the diagnosis he generates based on it. In this case, an accredited hosting of health data becomes necessary.
- Promote interoperability and standards especially around data exchange and semantic interoperability. We need to promote interoperability and open platforms, and move away from complex information silos where records and other data sit across multiple systems. For instance, our Nokia connected devices come with an extensive and cloud enabled API ecosystem allowing more than 100 partners and clients to develop and deploy their own innovative applications & services as needed.
- Sustain government leadership. Digital health investments need to be enabled by committed long term funding and robust program management. This will give newly introduced digital health solutions time and support to be implemented and to scale up in phases, and also to integrate with existing systems and practices. The Broadband Commission Working Group on Digital Health, chaired by Nokia and the Novartis Foundation, convened leading digital health experts from governments, international and non-governmental organizations, academic institutions and the private sector for the purpose of producing a report: Digital Health: A Call for Government Leadership and Cooperation between ICT and Health. This report documents the results of the exploration with a view to providing practical guidance on leadership governance and intragovernmental cooperation to leaders in health and ICT who wish to adopt a digital health strategy.
- The financial and regulatory framework. Today, billing for medical care does not sufficiently encourage early detection and home monitoring. Insurance for instance should put greater emphasis on reimbursing preventive care. Connected devices open the door to a new model of prevention. If today a disease treatment is reimbursed, it is conceivable to fund good health itself in the future. Lastly, sick patients and healthy people alike lack incentives to adopt prevention tools. sedentary lifestyle, smoking habits and lack of exercise increase the odds of cancer and cardiovascular diseases. In this context, a system rewarding healthy behaviors could be imagined.

